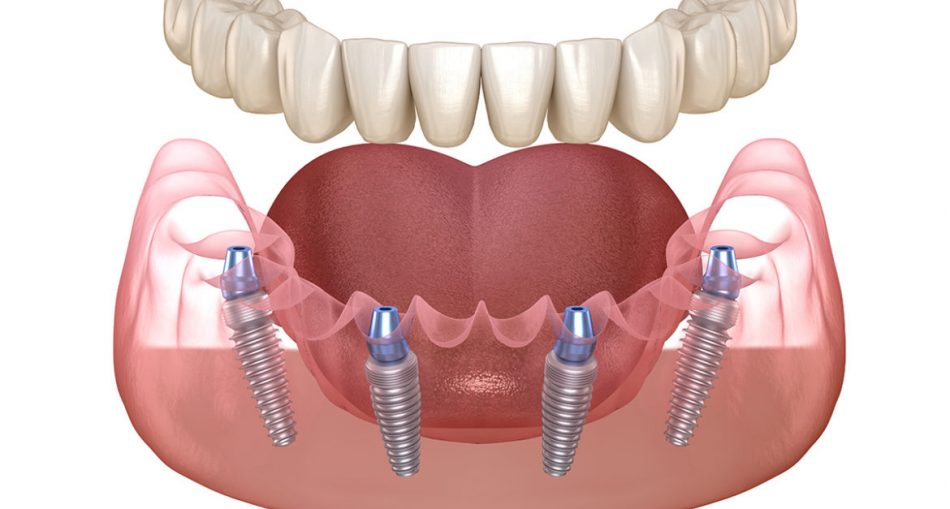
Dental implants are the modern surgical procedure used to remedy missing teeth. It can be considered as the link or bridge between the artificial teeth and the missing bone structure. Over time, it is expected that the dental implant will fuse into the regenerating bony structure of the gum. This process is termed osseointegration.
For osseointegration to take place seamlessly, the composition of the dental implant needs to be impeccable. Check out these types of bone grafts used in making dental implants.
1. Autograft
The autograft is the most common type of bone graft used in the dental industry. It is obtained from the patient’s body and classified as the autologous bone graft.
The procedure of obtaining this type of graft involves harvesting a long strip of periosteum, which is a layer covering the outer surface of bones. The periosteum contains osteoblasts, which are cells that synthesize new bone tissue. After extraction, it undergoes sterilization to eliminate any harmful pathogens that may affect its quality and safety for medical use.
The harvested periosteal tissue is then cut down into small pieces and implanted into an appropriate location in the jaw bone region. It will fuse with existing bone cells to create a stronger and more stable structure for holding dental implants.
This type of graft has many advantages over other bone grafts used in dentistry. Autogenous bone grafts are very effective in filling missing teeth and have a lower chance of bone rejection.
2. Allograft
Allograft is a derivative of the term allogeneic, which means it is obtained from a donor, not a part of the same species as the patient. It is also known as xenogeneic tissue and can be obtained from animals or humans.
The most commonly used source for allografts are cadavers or deceased donors. The deceased donors are organ donors or people who have died from natural causes. Note that the organ donor must be assessed for any diseases before being considered a candidate. Disease screening minimizes rejection chances.
Allografts used in dentistry are obtained from human cadavers and then sterilized using gamma radiation to eliminate any harmful pathogens that may affect its quality and safety for medical use. In order to maximize their potential, they are also freeze-dried before they are put into storage to maintain their stability and quality.
Allografts have many advantages over other types of bone grafts used in dentistry. They have a high success rate when used to fill missing teeth and can be more easily placed in small areas than other graft types.
3. Alloplast Bone Graft
Alloplast is derived from the Greek word “allows,” which means other. It is also known as alloplastic. Alloplast bone graft is made from synthetic materials similar to bone and can be used as a substitute for natural bone in animals and humans.
They are used as a substitute for natural bone when there is not enough space for the new bone to grow or when the natural bone does not work well with the body. Alloplast bones are made to look, feel, and behave like real bones, but they are not derived from the same source as real bones.
Alloplast bones can be made of different materials such as ceramics, polymers, or biocompatible metals such as titanium or cobalt chrome. The most common material used to create an alloplastic implant is a ceramic called hydroxyapatite which has a structure similar to natural human or animal bones.
4. Xenograft Bone Graft
Xenograft is derived from the word “Xeno,” which means foreign. It is also known as xenoplastic.
Xenograft bones are made from the bones of other animals or humans. They are used as a substitute for natural bone when there is not enough space for the new bone to grow or when the natural bone does not work well with the body. Xenograft bones can be made of different materials such as metals, ceramics, polymers, and biocompatible plastics such as titanium or cobalt chrome.
Conclusively, the process of getting a dental implant is daunting, but the results are worth it. Choosing the right dental implant type is crucial in smoothening the healing process and minimizing the chance of organ rejection.